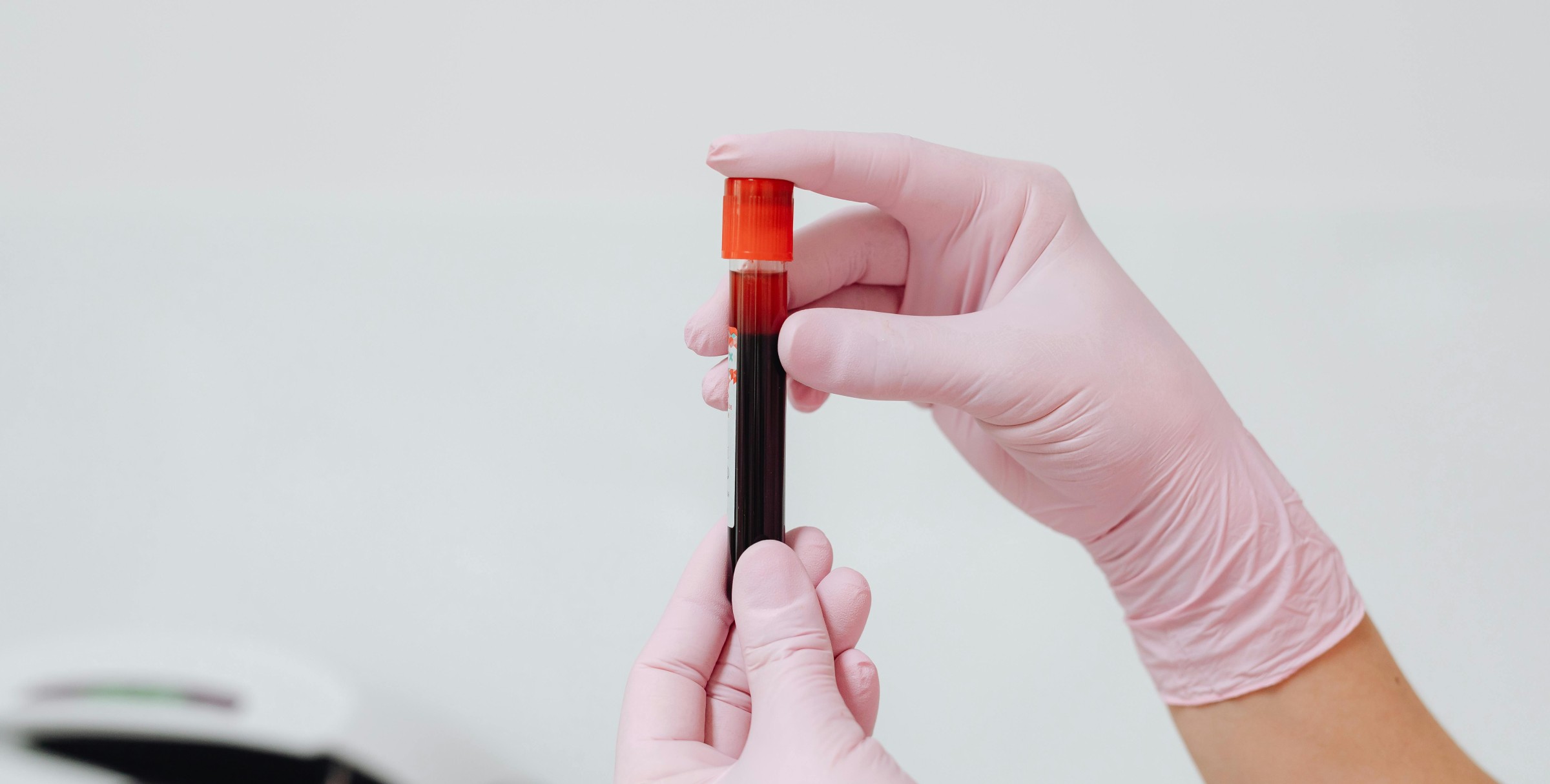
Many people believe that a routine blood test carried out during a general health check would automatically detect HIV. However, this isn’t the case. A normal blood test doesn’t screen for HIV, because routine panels focus on identifying general health markers, not detecting infections.
At Better2Know, our clinical dataset reinforces this reality: 100% of standalone HIV appointments use targeted antigen/antibody (Ab/Ag) or PCR diagnostics, not standard blood work. This unmistakably confirms that accurate HIV detection requires specialist testing—never routine blood panels. Keep reading to find out more.
What does a “normal” blood test include?
Standard blood tests typically assess:
- Red blood cell, white blood cell, and platelet levels
- Kidney and liver function markers (including urea, electrolytes, and protein)
- Cholesterol and glucose levels
- Thyroid-stimulating hormone levels
These markers help your doctors assess whether you may have conditions like hypothyroidism, cardiovascular disease, diabetes, and anaemia.
Would a normal blood test detect HIV?
While these blood test markers help doctors evaluate general health, they don’t identify anything you would need to diagnose HIV. Routine tests are not designed to detect viruses.
Standard blood panels don’t look for HIV. Unless your healthcare provider has a reason to test for a particular infection, it probably won’t be detected.
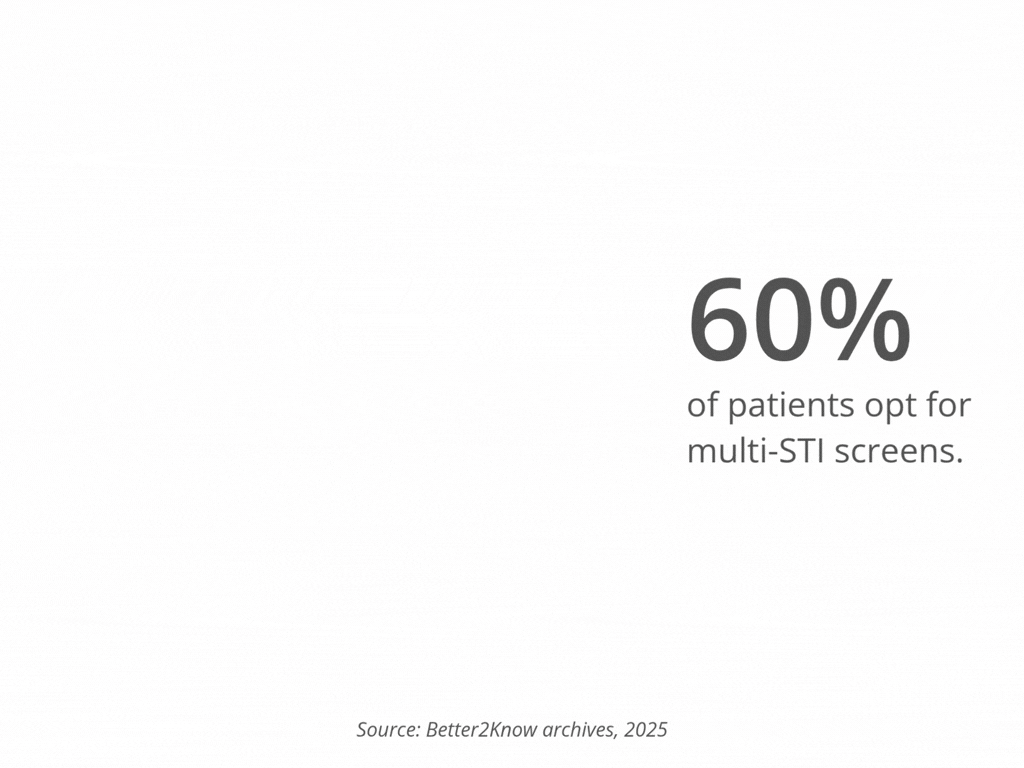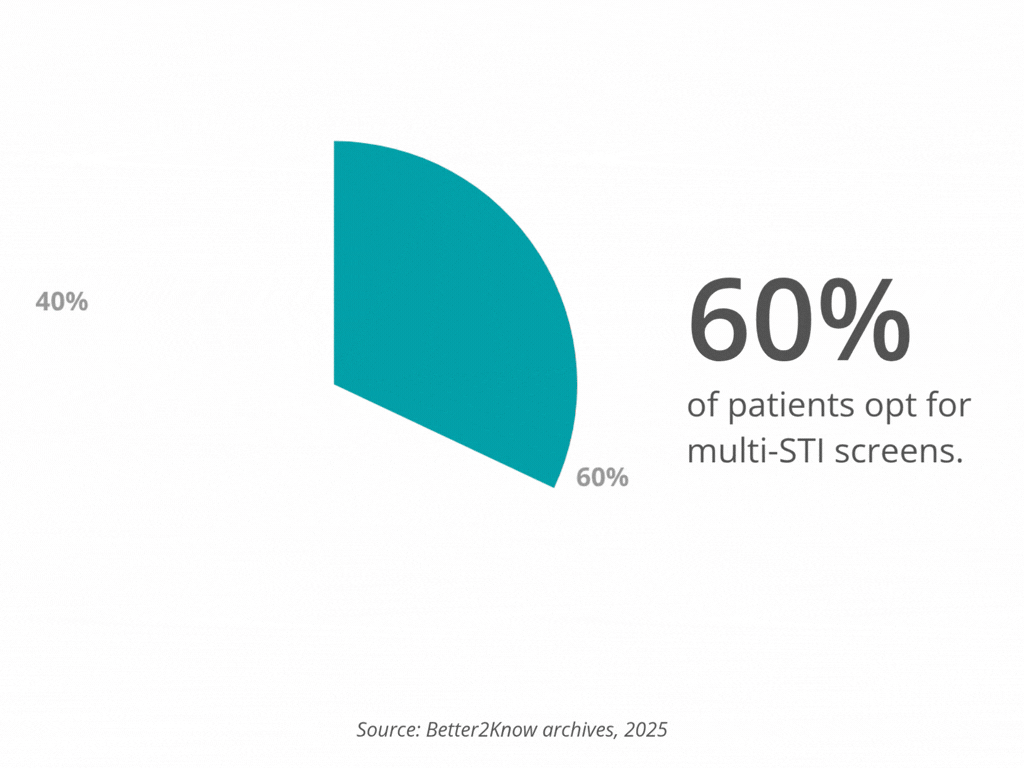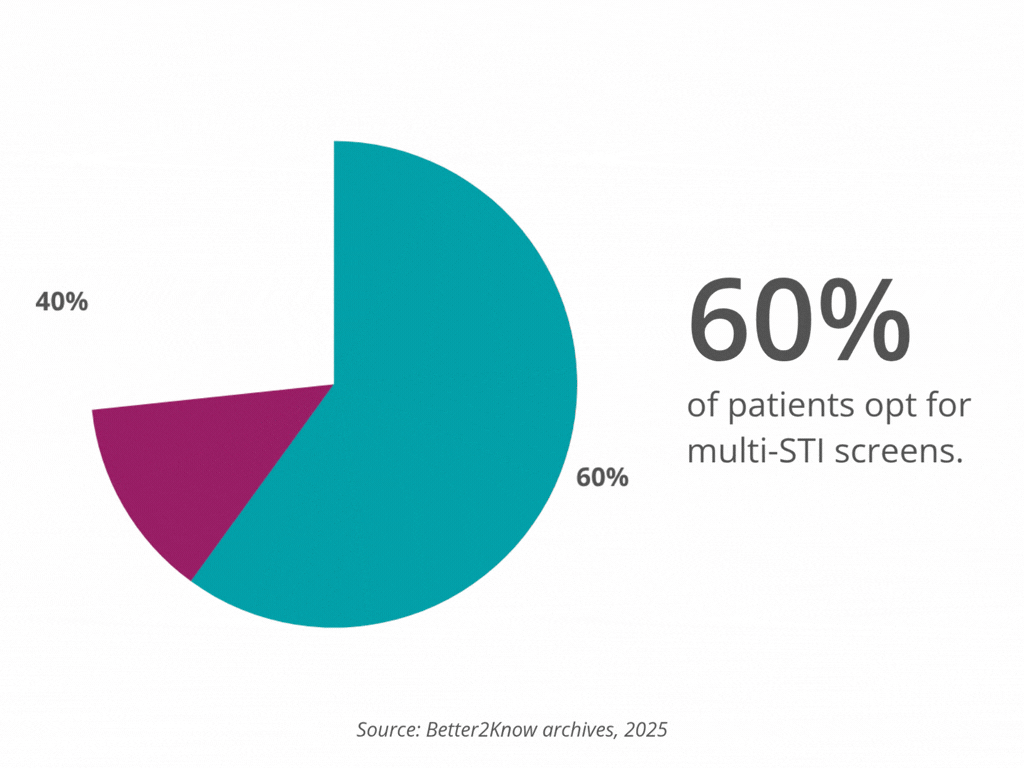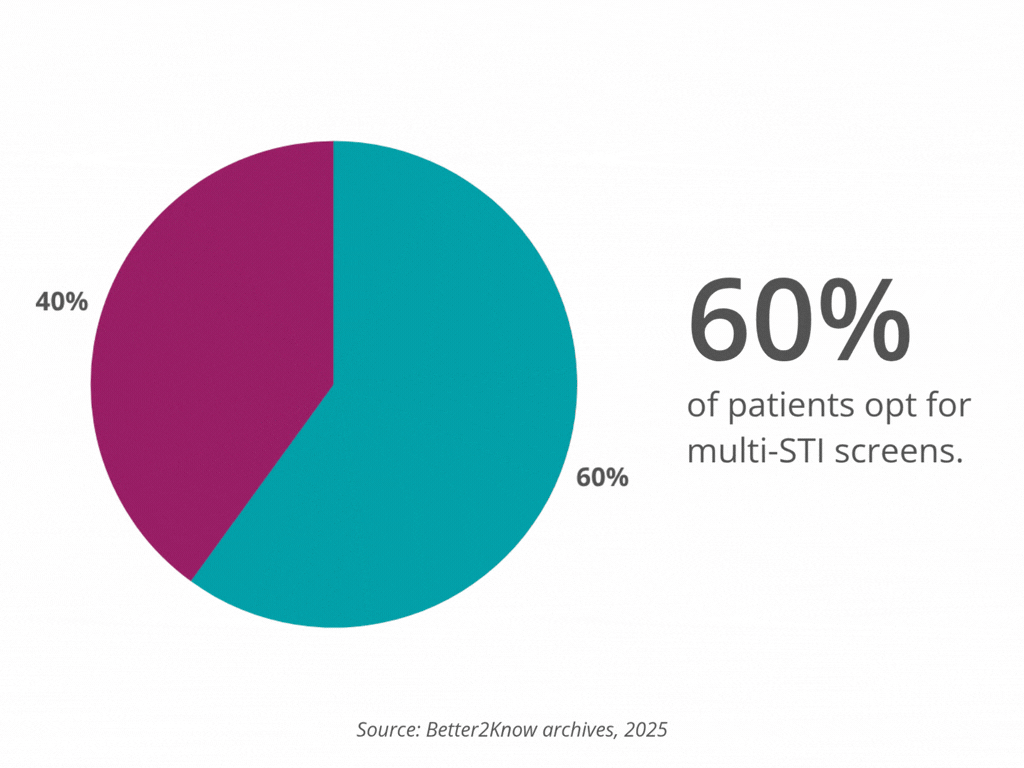
This is why most patients need a special test for HIV. Nearly 60% of patients choose high‑tier comprehensive STI panels, precisely because standard blood tests—even thorough GP panels—don’t include HIV screening. This aligns with clinical guidance in most countries that HIV testing must always be deliberately ordered.
Why do we need a special test for HIV?
To detect HIV, laboratory testing must focus on one or more of the following:
- HIV antibodies: Produced by the immune system in response to infection.
- The p24 antigen: A viral protein detectable 10–20 days after infection in 4th‑generation tests.
- HIV RNA (PCR / NAT Tests): Directly detects viral genetic material 10 days after the infection.
These markers are almost never included in general blood panels.
Real world testing behaviour supports Better2Know data
As an STI-testing company with global reach, Better2Know has more than a decade of experience. Our internal appointment dataset highlights three key trends:
100% of standalone HIV appointments utilise Ab/Ag or PCR tests
This shows that patients who specifically want answers for their HIV status understand they must use targeted tests—not routine blood panels.
Nearly 60% of clinic volume comes from high‑tier comprehensive panels
Patients select comprehensive STI panels because they know that standard GP blood tests do not cover HIV or other specific STI markers.
The average age of patients booking viral blood tests is mid‑30s
This is a demographic that typically understands health risks and recognises the need for lab‑based specialist diagnostics rather than general blood work.
These patterns mirror public‑health guidance: HIV diagnosis requires dedicated testing, not assumptions based on unrelated results.
Why relying on routine blood work isn’t a good idea
Depending on general blood tests for HIV detection can lead to:
- False reassurance, delaying diagnosis
- Potential onward transmission
- Missing early treatment opportunities, which improve long‑term outcomes
HIV is only detectable when the correct markers are analysed—and only specialist labs can perform these analyses accurately.
Final thoughts
A normal blood test will not show HIV. Only a specialist HIV test—antibody, antigen/antibody, or PCR—can detect the virus. Routine blood tests, even highly detailed ones, simply do not look for HIV markers.
To know your status with certainty, choose a dedicated HIV test. Click the button below to book an HIV test near you today.